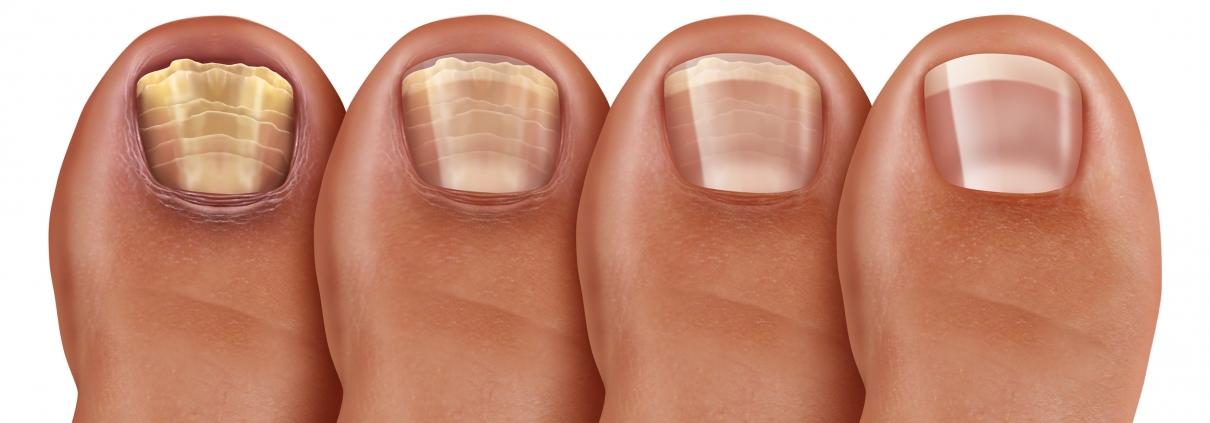
Fungal Nail Infections
Fungal nail infections, also known as onychomycosis, are a common and persistent condition affecting millions of people worldwide. This unsightly and often uncomfortable condition occurs when fungi invade the nails, leading to discoloration, thickening, and a gradual deterioration of the affected nail. While fungal nail infections are usually not a serious health concern, they can be bothersome, socially embarrassing, and may require proper treatment for resolution.
Causes
Fungal nail infections are primarily caused by various types of fungi, with the most common culprits being dermatophytes, yeast, and non-dermatophyte molds. These fungi thrive in warm, moist environments, making them more likely to affect toenails rather than fingernails. Some of the common causes and risk factors for developing a fungal nail infection include:
Poor foot hygiene:
Inadequate foot care and poor hygiene practices can create an environment conducive to fungal growth.
Warm and moist environments:
Swimming pools, communal showers, and damp footwear provide the perfect breeding ground for fungi.
Nail damage:
Any trauma or injury to the nail can make it more susceptible to fungal invasion.
Weakened immune system:
Individuals with compromised immune systems are more vulnerable to fungal infections.
Diabetes:
Diabetics are at an increased risk of developing fungal nail infections due to poor blood circulation and nerve damage in the feet.
Symptoms of Fungal Nail Infections
The symptoms of a fungal nail infection can develop gradually and vary in severity. Common signs of onychomycosis include:
Discoloration:
The affected nail may turn yellow, brown, or white.
Thickening:
The nail becomes thick and may be difficult to trim.
Brittleness:
The nail becomes brittle and prone to crumbling or splitting.
Distorted shape:
As the infection progresses, the nail may become misshapen or oddly contoured.
Debris buildup:
Debris, such as dead skin and fungal particles, may accumulate under the nail.
Separation of nail from the nail bed:
The infected nail may lift or separate from the nail bed.